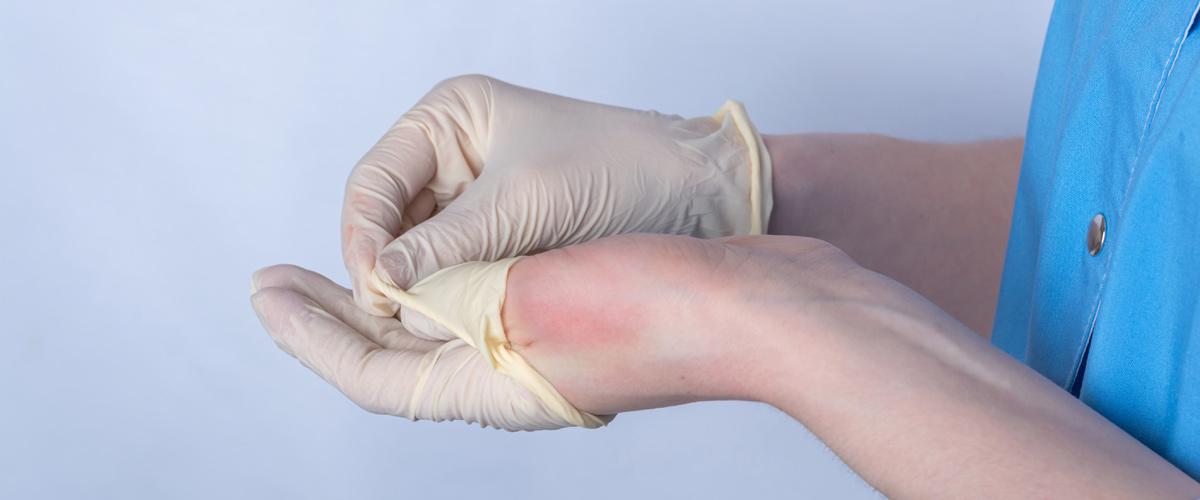
For healthcare professionals, hand hygiene and glove use are two key practices that help with preventing cross-contamination, and, consequently, healthcare-associated infections.
However, correct glove use is still a problem in many healthcare facilities. As a study carried out in a French university hospital shows, the rate of compliance with hand hygiene protocols after glove removal was only 51.5 per cent. Meanwhile, in 64.4 per cent of instances, gloves were not changed or removed when appropriate.1 It also goes without saying there are some misconceptions about gloves best practice—for example, the inaccurate idea that gloves can replace proper hand hygiene in healthcare settings. Therefore, infection prevention via glove hygiene has never been more important.
So what are the most common examples of glove misuse?
Broadly speaking, there are four common mistakes made by healthcare professionals concerning the application of approved gloving practices. These include:
- Failure to wear gloves when indicated: In such cases, healthcare professionals can facilitate cross-contamination when there is a risk of contact with bodily fluids, blood or pathogens, for example.
- Glove overuse: When healthcare professionals wear gloves in situations where glove use is not necessary (e.g. when moving a patient’s bed) this, more often than not, contributes to material waste. Moreover, there is no evidence that this practice helps with lowering the chance of cross-contamination.
- Gloves being used for longer than recommended: When should you change your gloves? This is still a difficult question for many. The failure to change gloves between patients, or missing an indicator for glove removal that could increase the chance of cross-contamination, is a prime example of glove misuse.
- Touching contaminated areas with gloves: Healthcare workers often touch potentially contaminated areas with gloved hands before proceeding to touch and examine patients. Therefore, once this happens, clinicians may be practicing with compromised or non-sterile gloves. This undoubtedly poses the risk of transferring pathogens from the environment in question to the patient.
Gloves best practice
Increasing the level of compliance to protocols for glove use and glove hygiene starts with education. You can characterise or complement this by:
- Routinely reminding healthcare professionals of the appropriate moments to perform hand hygiene, how to do so correctly, when to don and doff gloves, as well as how to ensure safe glove removal.
- Involving patients and loved ones in hand hygiene and gloving awareness activities, as this can potentially increase compliance. That is, it will create greater accountability amongst staff when patients are involved. Patients are more likely to actively enquire into whether their care provider has performed the right gloving and hand hygiene techniques.
- Resocialising staff, as a major part of facilitating compliance with sustainable and appropriate gloving practices has to do with their mindset and associated behaviours. For instance, there are two known barriers to proper glove use amongst healthcare professionals:
|
|
Gloves solutions that help
Leadership and setting examples are, therefore, important to change a healthcare professional’s perception. That is, both can be the difference between staff viewing glove wearing or use as burdensome, or embracing gloves as an effective source of protection for themselves and their patients.
In recognition of the usefulness of gloves, Medline offers a range of skin-friendly glove options to soothe and prevent allergic and irritant contact dermatitis. These skin-friendly options make life easier for healthcare professionals. Additionally, our nitrile examination gloves, for example, all have an accepted quality level (AQL) of 1.0, rather than the industry standard of 1.5. This means our production of gloves lowers the chance of pinholes occurring in a glove by up to 30 per cent. We carry a glove option for every wearer, setting and situation.
For more information, visit our online catalogue and explore our gloves and their protective properties, or browse our knowledge base.


Jeanne Verheyden
Exam Gloves Division, Medline Europe
Jeanne is a recent graduate from Vrije Universiteit Amsterdam, and received her Master’s degree right before joining Medline Europe as a Junior Product Manager. Her educational background is in international business and business administration, and during her studies she completed internships in Germany and the United Kingdom.
References:
1. Girou, E., Chai, S. H. T., Oppein, F., Legrand, P., Ducellier, D., Cizeau, F., & Brun-Buisson, C. (2004). Misuse of gloves: the foundation for poor compliance with hand hygiene and potential for microbial transmission?. Journal of hospital infection, 57(2), 162-169.
2. Wilson, J., Bak, A., & Loveday, H. P. (2017). Applying Human Factors and Ergonomics to the Misuse of Nonsterile Clinical Gloves in Acute Care. American Journal of Infection Control, 779-786.